When Do You Need Spine Surgery? Treatment and Recovery Guide
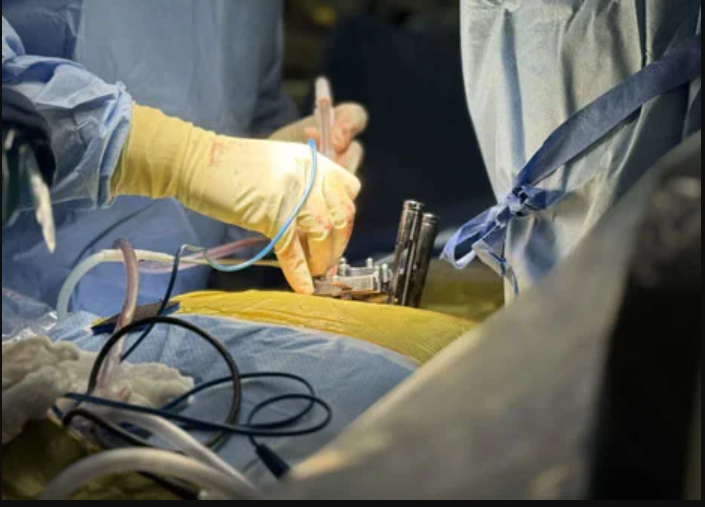
When back pain or neck discomfort turns from a nagging nuisance into a disabling condition, it may be time to consider spine surgery. Most patients first try conservative measures—physical therapy, anti inflammatory medication, epidural injections, and lifestyle adjustments—but when symptoms persist despite these efforts, or when imaging shows a structural problem that threatens nerves or spinal stability, surgery becomes a reasonable next step. Red flag signs such as progressive weakness, loss of bladder or bowel control, a rapidly worsening gait, or severe, unrelenting pain that interferes with sleep or daily activities are strong indicators that the spine’s anatomy is no longer able to protect the nervous system without operative intervention.
The decision to operate hinges on a thorough evaluation that includes a detailed history, a focused neurological exam, and high resolution imaging (MRI, CT, or dynamic X rays) to pinpoint the exact source of compression or instability. Common surgical indications include herniated discs that impinge on nerve roots, spinal stenosis that narrows the canal, spondylolisthesis or fractures that jeopardize alignment, and deformities such as scoliosis that compromise function. Surgeons weigh the benefits of each procedure—ranging from minimally invasive discectomy or micro decompression to more extensive fusion or artificial disc replacement—against potential risks like infection, blood loss, or adjacent segment disease.
If surgery is recommended, preparation starts well before the operating room. Patients are advised to quit smoking, optimize nutrition, manage chronic conditions (diabetes, hypertension), and often engage in pre habilitation exercises to strengthen core muscles and improve cardiovascular fitness. On the day of the operation, modern techniques such as intra operative navigation, neuromonitoring, and minimally invasive approaches help reduce tissue trauma and shorten hospital stays. Most elective spine surgeries now allow same day discharge or a brief overnight observation, with pain controlled by multimodal regimens that limit opioid use.
Recovery follows a predictable, phased timeline. The first few weeks focus on protecting the surgical site, gentle mobilization, and learning proper body mechanics to avoid re injury. Physical therapy is introduced early—often within 24–48 hours—to maintain flexibility and begin strengthening exercises tailored to the specific procedure. By six to eight weeks, many patients can resume light daily activities, while more vigorous tasks such as heavy lifting or high impact sports are typically delayed until three to six months, depending on the extent of the fusion or hardware placement. Regular follow up appointments with the surgeon and imaging studies ensure that the spine is healing as expected and allow timely adjustments to the rehabilitation plan.
Ultimately, Spine Surgery Flemington NJ is not a cure all but a targeted tool that restores the structural integrity of the spine, relieves nerve compression, and paves the way for functional recovery. By recognizing the warning signs, undergoing a comprehensive evaluation, and committing to a structured post operative program, patients can transition from chronic pain to a return of mobility and quality of life—often faster and more reliably than with prolonged non surgical therapy alone.





